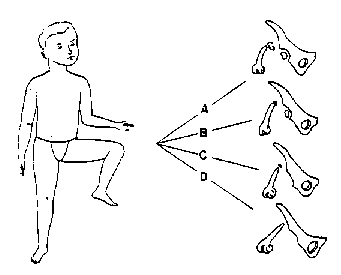
FIGURE 2 Schematic representation of the four radiographic subclasses of proximal femoral focal deficiency.
(Note from PFFDvsg Webmaster: Due to limited disk space and scanning problems, some of the Figures referred to in this document are not available online. My apologies for the inconvenience - hope to get them online soon.)
This is Section 1 of 5 from PFFD: A Congenital Anomaly, National Academy of Sciences, 1969.
GEORGE T. AITKEN, M.D.
Congenital anomalies of the proximal femur with or without involvement of
the iliofemoral joint have been observed and reported for many years (1).
The condition that has probably been best described and documented is congenital
or infantiIe coxa vara (3-5, 7, 9, 12).
As interest increased in the prosthetic treatment of certain skeletal limb
deficiencies, the existence of a group of partial deficiencies of the proximal
femur involving the iliofemoral joint became evident. These conditions were
poorly documented and unclassified. Neither the FrantzO'Rahilly (6) nor the
Hall (10) classification system for skeletal limb deficiencies, for
example, provides terminology for partial absence of either the femur or
the humerus. Hence, the designation "proximal femoral focal deficiency,"
or PFFD, was coined for this group of cases. This paper presents the clinical
and radiologic life history of this condition and outlines the author's
experiences and recommendations for treatment.
The clinical experience with this anomaly at the Area Child Amputee Center
in Grand Rapids, Michigan, may be summarized as follows: Of 35 cases considered
to January 1, 1968, there were 21 males and 14 females; of these 35 cases,
11 had right involvement, 19 left, and 5 bilateral. The typical clinical
picture is clearly shown in Figure 1. In severe cases, diagnosis can be made
by inspection. On the affected side there is a short femoral segment that
is flexed, abducted, and externally rotated. The tibia may or may not be
of normal length. Usually the sole of the foot on the affected side is about
at the level of the contralateral knee.
When serial x-rays of these patients are reviewed over a considerable period of time, it is possible to identify four radiologic subclasses of this condition (2). Figure 2 shows an artist's representation of the four radiologic subclasses.

FIGURE 2 Schematic representation of the four radiographic subclasses
of proximal femoral focal deficiency.
In Class A a head of the femur is present, together with an adequate acetabulum
and a very short femoral segment. Initially, there is no bony connection
between the segment and the head of the femur. At skeletal maturity in this
subtype a bony connection is present between the shaft ot the femur and the
head, neck, and trochanteric component. In most instances a pseudarthrosis
is evident at their point of connection, and this defect does not heal in
all inscances. It is possible that for this class the term PFFD is semantically
incorrect because basically there is no deficiency in the proximal femur
at skeletal maturity. There is simply inequality of femoral lengths and an
abnormal relationship between the head, neck, and trochanteric component
of the femur and its shaft, with severe subtrochanteric varus. This group
is included in PFFD because the clinical picture is essentially identical
with that of the other three groups.
The characteristics of Class B are the presence of a head of the femur and
an adequate acetabulum, together with a short, deformed femoral shaft, usually
with a small bony tuft on its proximal end. At skeletal maturity there is
no osseous connection between the femoral head and shaft. Cineradiographic
studies done on these children at skeletal maturity demonstrate that the
head does not move synchronously with motions of the shaft of the femur,
and, therefore, it is believed that there is no cartilaginous connection
between the shaft and head and neck segments.
In Class C the acetabulum is severely dysplastic. The head of the femur never
ossifies and it is believed that there is no cartilaginous model of the femoral.
The shaft of the femur is short with an ossified tuft at thc proximal end
of the shaft.
Class D is characterized by the absence of both the acetabulum and femoral
head; by a deformed, shortened femoral shaft; and by no proximal tufting
on the shaft of the femur.
It is important to recognize that although the clinical picture seems to
be identical in all of these cases, review of x- rays throughout the period
of a patient's pre- and postskeletal maturity demonstrates the presence of
four radiologic subclassifications. Further discussion of these types, with
a presentation of illustrative cases, follows.
CLASS A PROXIMAL FEMORAL FOCAL DEFICIENCY
An example of Class A PFFD is shown in Figure 3-A. This child's heel is about
level with the contralateral knee joint. The shaft of the femur is very short,
and there is associated fibular hemimelia. The flexion, abduction, and external
rotation deformities in this hip are not as characteristically extensive
as those found in most of these patients.
The radiograph in Figure 3-B was taken when the patient was one day old.
No acetabulum is evident and the shaft of the femur is very short. The femur
rides laterally in relationship to the ilium. The associated fibular hemimelia
on the same side can be observed.
At six years of age (Figure 3-C) the head of the femur is ossified. The shaft
of the femur is now riding above the acetabulum. A distal femoral epiphysis
is evident, together with an amorphous calcification of what is probably
a cartilaginous anlage of the greater and lesser trochanters and the base
of the femoral neck.
An x-ray of the same patient at twelve years and four months is shown in
Figure 3-D. The head, neck, and greater and lesser trochanters are now ossified,
but there is a pseudarthrosis between these components and the shaft. A severe
varus deformity is evident. It should be emphasized that this is a
subtrochanteric varus and is not a neck-shaft varus as is seen in typical
infantile coxa vara. It is this appearance that oftentimes leads observers
to mistakenly confuse Class A PFFD with congenital or infantile coxa vara.
Careful review of x-rays, such as those in Figure 3-D, in comparison with
those of typical infantile coxa vara, will demonstrate the difference in
the location of the varus deformity and will also demonstrate that the defect
in the PFFD is subtrochanteric, whereas the defect in infantile coxa vara
is at the level of the subcapital epiphysis.
At twenty years of age, ossification of the head, neck, and trochanters has
progressed (Figure 3-E), but a pseudarthrosis between the head, neck, and
trochanteric segments and the shaft persists. A severe, persistent
subtrochanteric varus is also present.
A representative clinical example of Class B is shown in Figure 4-A. On the
affected side there is a very short fempral segment, a short tibial segment,
and a deformed foot that extends to about the level of the opposite knee
joint. The child has numerous other limb deficiencies.
X-rays of this patient at eleven months of age (Figure 4-B) demonstrate that,
although an acetabulum is evident, the femoral head has not yet ossified,
and the shaft of' the femur is short, flexed, abducted, and externally rotated.
An associated fibular hemimelia is apparent on the same side.
The status of the same patient at ten years and nine months is shown in Figure
4-C. It is now evident that there is a head in the acetabulum and that the
head is ossified. The shaft of the femur still rides high, and at the proximal
end of the femoral shaft there appears to be a calcific tuft which may represent
a trochanteric apophysis. Cineradiographic studies in this case demonstrate
that there is no synchronous motion of the head with the shaft. This evidence
tends to substantiate the concept that there is no cartilaginous connection
between the femoral shaft and the ossified head of the femur.
Figure 5-A presents the characteristic clinical picture of Class C PFFD.
An x-ray of this patient at age two months (Figure 5- B) shows the very short
shaft of the femur, a moderately inadequate acetabulum, and fibular hemimelia
on the same side. The total leg length on the affected side is essentially
equal to the femoral segment on the contralateral side.
X-rays of the patient at eleven years and eleven months of age are shown
in Figure 5-C. The dysplasia of the acetabulum can be noted. There is no
ossification of the head of the femur on that side, and the shaft of the
femur rides proximal and posterior to the ilium.
The patient shown in Figure 6-A is a bilateral PFFD, Class D. An x-ray of
this patient at the age of seven years and five months is shown in Figure
6-B. Attention is directed to the obliquity of the lateral walls of the pelvis.
No ossification of the femoral heads has occurred and no acetabula are present.
The femora are very short and are flexed, abducted, and externally rotated.
No proximal tufts of ossification are evident on the femora.
X-rays of the same patient at eleven years and five months of age are shown
in Figure 6-C.
The differential diagnosis of this condition is generally not difficult.
Figure 7-A demonstrates a patient with a very short femoral segment, some
flexion, some abduction and external rotation, and marked inequality of leg
lengths. X-rays of this patient taken at one month (Figure 7-B) show that
she has a very short femoral segment, does have an acetabulum, and the femur
is laterally displaced with marked shortening as compared to the opposite
side. It is possible to confuse this condition with either a Class A or a
Class B PFFD at this age. Radiographs at age eight years and four months
(Figure 7-C) demonstrate that this patient does have infantile coxa vara.
This is a neck-shaft varus, with deformation of all of the components of
the head, neck, and trochantenc area, and shortening of the femur. This condition
represents idiopathic or juvenile or congenital coxa vara associated with
congenital shortening of the femur (8). This is an entirely different entity,
and the differential diagnosis between congenital coxa vara with a short
femur and PFFD Class A or B is generally best made by x-ray at approximately
one year of age.
The x-rays of a three-day-old patient (Figure 8-A) illustrate another possible
problem of differential diagnosis. This patient does have an acetabulum,
a short femur, and an anterolateral bowing of the femur in its midshaft.
X-rays of this child at fifteen months (Figure 8-B) demonstrate an adequate
acetabulum, a quite normal femoral head, proximal epiphysis, neck, greater
and lesser trochanters, and a quite normal femoral shaft except that it is
short and the anterolateral bowing at its midportion is gradually clearing.
It is interesting to note that this patient has an incomplete fibular hemimelia
on the same side. Figure 8-B demonstrates the shortening of the fibula on
the affected as compared to the unaffected side. This patient does have
leg-length inequality because of both femoral and tibial shortening. At the
present time there is no established classification for this combination
of congenital skeletal limb deficiencies. Patients with this condition may
often be confused with PFFD Class A or B at birth, but by six months of age
the x-rays clearly differentiate these two conditions.
Patients with proximal femoral focal deficiency, either unilateral or
bilateral, have a relatively high incidence of associated skeletal
limb deficiencies. For instance, in a study of 29 cases, 68.9 percent
had fibular hemimelia in the samelimb, and 51.7 percent had other skeletal
deficiencies in other limbs. From these figures it seems evident that
in many instances patients with PFFD fall into the category of the
multihandicapped child.
The biomechanical losses in children with lower-extremity skeletal limb
deficiencies can be characterized as:
1. Inequality of leg length
2. Malrotation
3. Inadequacy of proximal musculature
4. Instability of proximal joints
Patients with proximal femoral focal deficiency exhibit most of these
characteristics. They have inequality of leg lengths; there is malrotation
of the limb; there is inadequacy of proximal joints; and the proximal musculature
is also inadequate.
The concept of treating these children prosthetically is based on the
fact that prosthetic application will correct or at least improve many of
the biomechanical losses. Prostheses will equalize leg lengths. Prosthetic
fabrication and alignment can be used to correct or at least improve the
malrotation. By alignment and fabrication techniques it is possible to increase
the stability of the proximal joints by building in alignment stability.
The inadequacy of the proximal musculature is only minimally affected by
prosthetic applications.
If one accepts the concept of prosthetic correction of biomechanical losses
in this group of congenital skeleta1 limb deficiencies, then treatment must
be related to the nature of the defect and to the type of prosthetic restoration
that is desired.
If one first considers the unilateral cases, the possibilities of treatment are with either a below-knee or an above-knee type prosthesis. Except for possible hip surgery, treatment considerations and procedures are essentially the same for all unilateral types.
A unilateral case treated as a below-knee amputee will generally
require the Van Nes (13) 180-deg tibial rotational osteotomy. By such a procedure
the ankle joint becomes the knee joint, and the rotated foot becomes
the below- knee stump. This is a procedure which is recommended by many
authorities. This author has had no personal experience with it. In
selected cases there may be enough femoral length to fit the limb with a
below-knee prosthesis without rotation osteotomy, using the anatomical knee
joint. In this entity such cases are rare, however.
If one elects to treat a unilateral case as an above- knee amputee type,
then there are several mechanisms by which this type of management may be
accomplished.
Without surgical conversion, an above-knee type of prosthesis may be fitted
around the deformed foot. The knee joint is mounted below the foot, and by
prosthetic fabrication and alignment the axis of rotation is related properly
to the line of progression of the patient.
Such a procedure generally produces an above-knee socket with a rather
bulky distal end, but this bulk can be accommodated by clothing alterations,
and the fitting does provide very satisfactory functional restoration.
An alternative procedure is to ablate the foot by ankle disarticulation and
fashion a Syme's-type stump closure. This procedure produces an above-knee
type of stump of a more satisfactory shape and one which will permit at least
partial if not complete end-bearing. A standard knee joint is then attached
to the above-knee socket, and by alignment techniques the knee joint is properly
related to the line of progression of the patient. This fitting also produces
a very satisfactory functional result.
In association with ankle disarticulation, additional surgical conversion
procedures may be introduced. Specifically, arthrodesis of the knee will
produce a rnore stable stump s.keleton, and in selected cases is a desirable
procedure.
In the 30 cases of unilateral PFFD treated at the Area Child Amputee Center, surgical procedures used wer as follows: 15 ankle disarticulations, 6 knee arthrodeses, and 7 reconstructions about the hip.
The patient depicted in Figure 9-A presents the characteristic clinical
appearance of a unilateral PFFD. Prior to admission to the Area Child Amputee
Program the patient had been fitted with a shoe and skate that simply equalized
leg lengths (Figure 9-B). The patient and his family were not entirely satisfied
with his fitting. It was recommended that he be treated by ankle disarticulation
and fitting as an above-knee amputee, but he elected to be fitted around
the foot. In Figure 9-C the boy is shown wearing a nonstandard prosthesis
of a type which can be fitted around the foot of a surgically untreated PFFD.
The knee joint is mounted underneath the heel. A standard shinpiece and a
SACH foot are used. Figure 9-D presents a close-up view of the hinged split
socket of laminated plastic held in place by Velcro straps.
Figure 10-A shows another child with unilateral PFFD. Initial prosthetic
fitting was simply to equalize leg lengths by means of an ischial-bearing
brace (Figure 1 0-B). Later, ankle disarticulation with construction of a
Syme's-type flap was accomplished (Figure 10-C). The patient was subsequently
fitted with a nonstandard above-knee type of prosthesis (Figure 10-D). Early
suspension was accomplished by an over-the-shoulder strap; later, simply
by a Silesian bandage. Standard knee joints, a standard shankpiece, and a
SACH foot are incorporated in the prosthesis.
Figure 11 shows a patient treated by ankle disarticulation and then, in order
to give him a more stable above-knee stump, knee arthrodesis.
When knee-joint arthrodesis is to be performed, the time to do this surgery
must be carefully selected so that the growth potentials of the proximal
tibial and distal femoral epiphyses are not destroyed at too early a date.
Miscalculation may produce an above-knee type of stump which is too short
for satisfactory prosthetic fitting. Knee-joint arthrodesis helps to correct
the flexion, abduction, and external rotation deformities of the hip. These
patients can be fitted with standard quadrilateral suction sockets, and
end-bearing can sometimes be used if the Syme's-type flap covering the ankle
disarticulation has been properly constructed.
In properly selected cases, reconstructive surgical procedures about the
hip joint to improve hip stability and thus facilitate maximum usage of hip
musculature are desirable. As previously emphasized, only Class A and
Class B PFFD cases have adequate acetabula and femoral heads. Hence, it is
only in these two groups that reconstructive surgery about the hip would
seem to be indicated. It is, therefore, essential that the four radiologic
subclasses of the basic clinical entity be clearly differentiated and that
hip surgery be carried out only in those cases where ther is afemoral head
and an acetabulum.
Although the author has himself had experience with the procedure, the best example of reconstructive hip surgery he has seen was a case of the late Dr. Oskar Hepp of Muenster, Germany (11). Figure 12-A shows the preoperative x-ray revealing a typical Class A PFFD. Dr. Hepp simply explored the area and with sharp dissection removed all of the cartilaginous model that existed between the shaft and the head. He then placed the shaft directly underneath the head and held it in 180 deg of valgus until healing occurred. Figure 12-B shows the result three years after surgery.
It is the author's contention that a patient with bilateral PFFD should not
be fitted as a below-knee amputee because bilateral Van Nes rotational
osteotomies are not indicated. A patient with bilateral PFFD can walk
comfortably and adequately on his own feet. His condition makes him a
disproportionate dwarf, but in the confines of his own home he is very
apt to ambulate in this manner because he is more stable and comfortable.
If one attempts to treat him as a below-knee type by surgical conversion,
his ability to ambulate without prostheses is destroyed. If one attempts
to fit him as an above-knee amputee and ablate the feet, carry out knee
arthrodeses, and do reconstructive surgery about the hip, he is again prevented
from ambulating without prostheses. It is the author's firm belief that,
in the bilateral case, one should never destroy the aptients ability to ambulate
without prostheses. If one accepts this concept, the the prosthetic treatment
of children with bilateral PFFD is to fit around the feet, mount the knee
joints under the feet, and treat the patient as a bilateral, nonstandard
above knee amputee. Knee arthrodesis is not indicated in these cases because
it interferes with nonprosthetic ambulation.
It should be emphasized that the bilateral PFFD's observed in the Area
Child.Amputee Center have been, with one exception, all Class D cases. Hence,
these patients had no acetabula and no femoral heads. Reconstruction about
the hip in these cases is probably not indicated. Moreover, if one accepts
the concept that these patients desire to walk on their own feet (at least
within the confines of their own homes), then arthrodesis of the knees in
the presence of severely unstable hips will not improve function.
The patient shown in Figure 13-A has bilateral PFFD. Since these patients
are capable of walking on their own extremities at all times, prosthetic
application simply makes it possible for them to be as tall as their
contemporaries if they are willing to become "stilt-walkers." Figure 13-B
shows this patient with her prostheses. She accommodated to stilt-walking
and preferred this method of ambulation out of the confines of her own home.
She is shown as a midteenager in Figure 13-C. She still walks as an above-knee
amputee with her prostheses fitted around her feet. However, she reverts
to walking without her prostheses in the confines of her own home, where
the disproportionate dwarfism is not the cosmetic problem that it is in
public.
Figure 14-A presents a patient with bilateral PFFD who was first seen in
infancy in the late 1930's. At that time, the concept of prosthetic application
to improve function and cosmesis in bilateral PFFD patients was not recognized.
When this patient was approximately fifteen years old, she was recalled and
an attempt was made to fit her with stilttype prostheses, which she rejected.
She had adjusted to her disproportionate dwarfism and preferred the stability
of walking on her own legs and feet to the instability of walking on the
stilt-type prostheses. Figure 14-B shows this patient, now an adult, with
her normal son standing beside her. Had this patient been treated by bilateral
ankle disarticulation she would have been compelled permanently to walking
with prostheses. Given the choice of being a disproportionate dwarf or a
stilt-walker, or combining these states, she has had a more satisfactory
functional existence. In this instance, she was functional to the point that
she has been able to rear a child.
Another bilateral PFFD, shown in Figure 15-A, has associated upper-extremity
amelia. He ambulates independently on his own feet. Most patients with bilateral
above-knee-type prostheses require some form of external support. The author's
figures indicate that 51.7 percent have other limb deficiencies in addition
to PFFD. Had this patient been treated by ankle disarticulations he would
have been a poor bilateral above-knee prosthetic walker because he has only
one upper extremity to utilize for crutch or cane support. This boy was fitted
around his feet as an above-knee amputee (Figure 15-B). This gives
him normal height if he desires it, but it lets him be independent on his
own feet when he desires to be that way.
The patient shown in Figure 16-A had multiple operative procedures in attempts
to correct his deformities, and some of these procedures were done about
the hip joint. The purpose of these operative procedures was to stabilize
the hip joint by iliofemoral arthrodesis in order to increase stability at
the hips. An x-ray of the patient's pelvis (Figure 16-B) reveals multiple
internal fixation devices. He has ended up with his hips fixed by scar or
bony arthrodesis in flexion, abduction, and external rotation, and this fixed
position makes it impossible for him to walk without a walker type of external
support. He has associated upper-limb anomalies. It is the author's contention
that such surgery has not improved this boy's function.
Proximal femoral focal deficiency is a congenital skeletal limb deficiency involving the proximal end of the femur and, in most instances, the iliofemoral joint. The life history of this anomaly is fairly well known and documented. Serial study of radiographs of these cases indicates that there are four radiographic types. The biomechanical loss in these cases can be categorized as inequality of leg lengths, malrotation, instability of proximal joints, and inadequacy of proximal musculature. Prosthetic application can correct the major biomechanical losses by equalizing leg lengths, correcting malrotation by prosthetic fabrication and alignment, improving the stability of the proximal joint by alignment and fabrication techniques, and at least ameliorating the inadequacy of proximal musculature by prosthetic stability. Classes A and B may obtain improved function by surgical reconstruction about the hip joint. Patients with unilateral PFFD may be treated as below-knee or above- knee amputation-type patients. If they are treated as below-knee patients, they will require a Van Nes 180-deg tibial rotational osteotomy. If they are fitted as above-knee amputees, above-knee prostheses may be fitted around there deformed feet with a knee joint mounted below the foot, a standard shankpiece, and a SACH foot. The alternative is ablation of the foot by ankle disarticulation and the fashioning of a Syme's-type closure. Supplemental knee arthrodesis may be of value. In the bilateral cases, it is the author's contention that patients should be fitted around the deformity so that their feet and knees are preserved in order that they may retain their ability to stand and walk without their prostheses if they so desire, and may have the option of utilizing prostheses for cosmetic restoration as much or as little as they desire.
FIGURE 1 Clinical picture of proximal femoral focal deficiency with
associated fibular hemimelia The short femoral segment is flexed, abducted,
and externally rotated. The equino-valgus deformity of the foot is typical
of fibular hemimelia
FIGURE 2 Schematic representation of the four radiographic subclasses of
proximal femoral focal deficiency.
The courtesy of Chester A. Swinyard, M.D., in releasing for publication some ot the illustrative material in this monograph is appreciated.
1. Aitken, G. T. Amputation as a treatment for certain lower extremity
congenital abnormalities.
J. Bone Joint Surg., 41A (7):1267-1285, 1959.
2. Aitken, G. T. Proximal femoral focal deficiency. In
Limb Development and Deformity: Problems of Evaluation and
Rehabilitation. Springfield, Illinois: Charles C Thomas, Publishers, 1969.
3. Amstutz, H. C., and P. D. Wilson, Jr. Dysgenesis of the proximal
femur (coxa vara) and its surgical management. J. Bone Joint Surg. 44A(1):1-24,
1962.
4. Babb, F. S., R. K. Ghormley, and C. C. Chatterton. Congenital coxa
vara. J. Bone Joint Surg. 31A(1):115-131, 1949.
5. Fairbank, H. A. T. Infantile or cervical coxa vara, pp. 225-24 l.
In The Robert Jones Birthday Volume. London: Oxford liniversity
Press, 1928.
6. Frantz, C. H., and R. O'Rahilly. Congenital skeletal limb deficiencies.
J. Bone Joint Surg. 43A(8):1202-1224, 1961.
7. Golding, F. C. Congenital coxa vara. J. Bone Joint Surg. 30B(1):161-
163, 1948.
8. Golding. F. C. Congenital coxa vara and the short femur. Proc. Roy.
Soc. Med. 32:641-648, 1939.
9. Gould, G. M., and W. L. Pyle. Anomalies and Curiosities or Medicine.
New York: The Julian Press, inc., 1896.
10. Hall, C. B., M. B. Brooks, and J. F. Dennis. Congenital skeletal deficiencies
of the extremities: Classification and fundamentals of treatment. J.A.M.A.
181:590-599, 1962.
11. Hepp, 0. Personal communication.
12. Mital, M. A., K. S. Masalawalla, and M. G. Desai. Bilateral congenital
aplasia of the femur. J. Bone Joint Surg. 45B (3):561-565, 1963.
13. Van Nes, C. P. Rotation-plasty for congenital defects of the femur. J. Bone Joint Surg. 32B:12, 1950.
This is Section 1 of 5 from PFFD: A Congenital Anomaly, National Academy of Sciences, 1969.